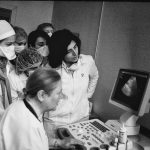
Georgian Solution for a Post-Soviet TB Program: Can Integration into Primary Health Care Improve TB Care?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care. Since 2005, Georgia has emerged as the regional leader in decentralizing TB services and implementing country-wide directly-observed treatment (DOTS) coverage in line with the major components of the international Stop TB strategy.
Through several waves of healthcare reforms, former stand-alone TB dispensaries across the country, except the major cities, have become physically integrated into Primary Health Care (PHC) centers which are now owned by private providers who contract TB doctors (in Georgia—only phtysiatrists) and DOT nurses to deliver TB services as part of the TB state program. Universal access to diagnostic and treatment services is ensured and facilitated by demand-side incentives and robust monitoring and evaluation practices which are reflected in high 83% treatment success rate for all new and ralapse cases registered in 2014.
Photo credit: Sophio Gokhelashvili
However, the most challenging drug-resistant TB (DR-TB) remains Georgia’s Achilles heel, as no more than 43% of patients completed treatment successfully in 2013, and every third of them interrupted treatment in the past three years.
The latest TB adherence report in Georgia found that almost half of drug-resistant patients are lost to follow-up already by the 8th month of treatment. This figure is not surprising if we put ourselves in the shoes of patients who have to travel to TB units six days a week for at least 18 months (DOTS units are not within walking distance for most patients, and flexible programs like Video-Observed Treatment (VOT) have limited coverage under pilot schemes). Poor management of side effects from anti-TB drugs also contributes to dropouts. Ironically, hospitalized patients in the Tbilisi TB center are better off as they have access to medical specialists who manage their adverse reactions. In rural areas, patients do not always use general healthcare services, required to complement their TB treatment. Despite structural integration of TB services into primary care facilities, the vertical TB program is not linked with the PHC services. As a result, TB patients are not well informed about certain free general care services under the UHC program, and they avoid additional expenses associated with seeking specialists on their own. Grossly underpaid, TB doctors are discouraged to meticulously engage in holistic patient care which are required to support drug-resistant patients. Budding medical students see no appealing career path in phthisiatry either, so the numbers of TB specialists are declining. The shortage is already felt in some regions where only one TB doctor serves several districts. Lack of coordination between the TB program and primary care services exacerbates sub-optimal organization of TB services. While a TB doctor, family doctor and other specialists often occupy the same facility, they do not share patient records and rarely cross-manage co-morbidities. As a result, formal decentralization of TB services in rural and semi-urban areas falls short of providing country-wide patient-centered care: if you want to receive quality treatment, better go to the Tbilisi TB center. Although the government is committed to addressing these shortcomings,
it is unclear whether a vertical program can cope with these challenges, even with further investments.
Drug-resistant patients require a flexible chronic care model which is more appropriate for the primary care level. Moreover, the declining TB epidemic will eventually phtysiatry redundant and the costly TB center unsustainable. This raises the question: how to uphold the benefits of holistic care offered at the primary care level without losing the capacity of a strong infection control vertical program? How much responsibility for TB care can family doctors successfully assume? Georgia has decided to test the feasibility of integrating TB services into primary care. Currently, I am here studying how such model could work.
I conducted a literature review on TB case management at the primary health care (PHC) level and found that
integration of specialized TB services into general practice is now understood to be essential to patient-centered care.
Conceptually, PHC centers which are operated by a family doctor or general practitioner can be ideal sites for participating in TB control as they are geographically close to patients, can deal with a broad range of health conditions, and ensure confidentiality which is crucial for stigmatized TB patients. However, it does not mean that all family doctors are expected to fully treat TB and assume all responsibilities of TB specialists. A quite successful model of TB care features multidisciplinary team case-manegement, practiced in countries like Norway, UK, and the US, which have 50% fewer patients lost to follow up, than Georgia (data on Norway, UK, USA). Particularly designed to support patients with more complex needs, multidisciplinary teams include a mix of prefossionals such as a TB lead physician (general practitioner), case manager, infectious disesase doctor or other TB specialist, as well as a social worker, peer supporter, psychiatrist, and legal services representative. However, all countries have different history of TB epidemic and TB care management, making it impossible to simply adopt more successful models. Reforming vertical TB programs is still new, so countries learn by trial and error. Several countries in the EECA region started engaging family doctors in TB control beyond case identification and diagnostic referral, enabling them to provide DOTS in Uzbekistan, Romania and Moldova, and even allowing family doctors in Serbia to prescribe anti-TB drugs. Unfortunately, there is little documented evidence from international practices in shifting TB service provision from specialized care to general practice. Country reports and project evaluations usually discuss normative dimenstions of interventions, and document specific inputs and outcomes, but rarely go in depth on the rationale behind certain programmatic choices and on-going operational challenges.
We need more present-day evidence that fills the gaps of publication delays to inform policy decisions promptly.
In March, Georgia launched a 48-month Results-Based Financing (RBF) scheme for tuberculosis care, hoping to incentivize family doctors and TB specialists (phtysiatrists and DOT nurses) to collaborate in patient-centered TB management. It is expected that giving family doctors more responsibility for TB case management would bring health services closer to patients. Engagement of family doctors would also stimulate the creation of linkages between TB doctors and other health specialists, ensuring that patients receive quality health services along the continuum of care. This program is currently in the design stage. Selective RBF schemes for TB have been introduced in Kazakhstan and Moldova, and pilots are underway in Armenia and Romania. Little impact evidence is documented in this area as well, and I hope the blog will encourage more timely and informal international knowledge exchange.
What we understand so far is that countries have to deal with a number of health system and individual barriers related to health financing, medical beliefs and attitudes, as well as communication and leadership skills of healthcare managers at all levels of care. Several studies consistently note that proper coordination of TB case management activities did not happen when family doctors and TB specialists were assigned new roles without ensuring that they understand and accept them. Other studies warn us not to underestimate the importance of healthcare managers whose leadership and motivation are as crucial as the competency of medical specialists. Moreover,
designing a flawless intervention from a system’s perspective will not ensure acceptability and uptake of the innovation by health professionals and patients.
Studies in Brazil, Turkey and India note that health workers’ resistance to changing professional practice was one of the major impediments to smooth TB integration in general practice. Hierarchical professional relationships among medical specialists are common in vertical programs such as here in Georgia. To establish successful case management of TB in primary care, healthcare managers are faced with the challenging task of ensuring that family doctors do not feel dominated and undervalued by TB specialists and, on the other hand, they do not underestimate their capacity to take new responsibilities and make a positive change for TB patients. The bottom line question is:
HOW to ensure harmonious task shifting when it requires not only acquisition of new skills and competencies but ultimately a paradigm shift for healthcare workers and patients?
Lessons from other countries suggest that functional information sharing systems and strong linkages between healthcare professionals at all levels of care become crucial to successful integration. Delayed or incomplete patient records disempower healthcare providers as they experience inefficiency of the system, caused by duplication of activities and endless paperwork. But again, HOW to establish these linkages? What crucial inputs should not be overlooked, especially once financial and regulatory mechanisms are aligned with the intended model of care? How to establish clear guidelines for the members of TB care team, while accommodating individual patient needs and variations in health resources across the country? How to ensure personal accountability while rewarding team performance?
Even though a lot of unanswered questions remain, the momentum for sustainable transformation is there, giving us an excellent opportunity to exchange the newest evidence and accelerate global progress towards TB eradication. As we will be following how Georgia deals with these challenges, we encourage you to share with us your experiences integrating TB services in the primary care, including innovative solutions and treatment models that promote patient-centered care.
Latest News
Integrated Bio-behavioral surveillance and population size estimation survey among Female Sex Workers in Tbilisi and Batumi, Georgia, in 2024
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation at Eighth Global Symposium on Health Systems Research (HSR2024)
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
“The Informatics and Data Science for Public Health: Sustainment Plan for Skilled Labor Force Development”
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Janina Stauke from the London School of Hygiene and Tropical Medicine shares her internship experience
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Jolly Mae Catalan fromUniversité Libre de Bruxelles shares her internship experience
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgia’s Journey to Integrating Rehabilitation Services into the Health System: Insights and Lessons
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Report on Rehabilitation Data Flow in Georgia’s Health Information System
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgia: a primary health care case study in the context of the COVID-19 pandemic
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Assessment of the Quality of Maternal and Neonatal Services in Montenegro
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgian state rehabilitation program: implementation research study report
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Strengthening Health Systems for Accessible Rehabilitation Services in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Linked’s workshop on HPV vaccine introduction and scale up, held on July 11-12th, 2023
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Training program focusing on interdisciplinary evaluation of rehabilitation interventions and patient outcomes
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Unlocking Success Through Learning: Workshop on Strengthening HR Capacity and Performance Management in Immunization
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Promote evidence-based policies in the pharmaceutical sector by generating evidence and fostering civic engagement
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF and the Results for Development / Accelerator combined their expertise to co-author an insightful blog, shedding light on Georgia’s commendable efforts to overcome limited data challenges and develop evidence-based policies for financing rehabilitation services
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Culminating event – Building Institutional Capacity for Health Policy and Systems Research and Delivery science (BIRD) in six WHO Regions
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Report on Phased (Stepwise) Plan for the Capability Development of the Priority Rehabilitation Services
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Promote evidence-based policies in the pharmaceutical sector by generating evidence
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Mandatory Vaccination and Green Passes – Review of International Experience
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Sustaining Public Health Gains after Donor Transition: What can we learn about Georgia?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation at Seventh Global Symposium on Health Systems Research (HSR2022)
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation at Global Symposium on Health Systems Research
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Study report: Adaptations made in TB response during Covid-19 pandemic in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
New case study: Sustaining effective coverage with Opioid Substitution Therapy (OST) in Georgia in the context of transition from external assistance
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
New case study: National Immunisation Program Transition from external assistance
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
“Strengthening Health Systems for Accessible Rehabilitation Services in Georgia” – Workshop
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Strengthening the Delivery of Immunisation Services Through PHC Platforms-Workshop
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
New Paper: A transdiagnostic psychosocial prevention-intervention service for young people in the Republic of Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Vaccine Procurement and Supply for the Expanded Program of Immunization in Kazakhstan
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Prevention of Addiction and Mental Health in Adolescents in Georgia (PAMAd) – Workshop
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Data Analysis and Synthesis Workshop – analyzing the implications of the structure of Georgia’s private healthcare market for quality and accessibility
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
External Reference Pricing Policy: A Possible Pharmaceutical Price Regulation Policy in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Paper: Soviet legacy is still pervasive in health policy and systems research in the post-Soviet states
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Article: How do participatory methods shape policy? Applying a realist approach to the formulation of a new tuberculosis policy in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Bundled Payment Methods: An Alternative Payment Method to Contain Healthcare Costs in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
HOW TO MAINTAIN ROUTINE IMMUNIZATION DURING COVID-19? EXPERIENCES FROM ARMENIA, GEORGIA, AND UZBEKISTAN
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
GEORGIA COVID-19 VACCINE COMMUNICATIONS CAMPAIGN TO ADDRESS HESITANCY ISSUES
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgian Healthcare Barometer XIV Wave The analysis of financial stability and risks in healthcare
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
We are pleased to announce that The Sixth Global Symposium on Health Systems Research (HSR2020) has opened
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Discussing interim results of research project: Prevention of Addiction and Mental Health in Adolescents in Georgia (PAMAd)
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Effects of Pay for Performance on utilization and quality of care among Primary Health Care providers in Middle and High-Income countries
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CAN SOCIAL MEDIA MONITORING LEAD TO IMPROVED PERCEPTIONS ABOUT IMMUNIZATION?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The first phase of the joint fellowship program of the Curatio International Foundation and the Knowledge to Policy Center (K2P) at the American University of Beirut has been successfully implemented
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
LNCT WEBINAR: Incremental Costs of Routine Immunization, Campaigns, and Outreach Services During COVID-19
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
LNCT Webinar: Assessing Bottlenecks to Adequate and Predictable Vaccine Financing
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
LNCT WEBINAR: Designing Behavioural Strategies for Immunization in a Covid-19 Context
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Concentration and fragmentation: analyzing the implications of the structure of Georgia’s private healthcare market for quality and accessibility (ConFrag)
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
#COVID19 – Evidence and Policymaking: Personal Reflections from an LMIC Setting
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
LNCT Webinar: Key Considerations for Integrating Immunization with Other Primary Health Care Services
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgia Sharing knowledge to Armenia to strengthen immunization legislation
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Project on “Technical Assistance Using Modern Technology for TB Prevention, Diagnosis, and Increased Quality Treatment” was closed
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Dialogue on Pharmaceutical pricing policies to improve the population’s access to pharmaceuticals in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
LNCT Webinar: Implementing a High Performing Immunization Program within the Context of National Health Insurance: What can we Learn from Thailand?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
LNCT Webinar: Strengthening Public-Private Engagement for Immunization Delivery
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Implementing new research: Prevention of Addiction and Mental Health in Adolescents in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgia’s introduction of the Hexavalent vaccine: Lessons on successful procurement and advocacy
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgia Primary Health Care Profile: 6 Year after UHC program introduction
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
HSR2020: RE-IMAGINING HEALTH SYSTEMS FOR BETTER HEALTH AND SOCIAL JUSTICE
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CALL FOR MENTEES: PUBLICATION MENTORSHIP FOR FIRST-TIME WOMEN AUTHORS IN THE FIELD OF HPSR
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
A pilot of a new intervention launched to Improve adherence to TB treatment and its outcomes in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Training for epidemiologists and health workers on TB contact tracing new guideline
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Workshop on using modern technology for TB prevention, diagnosis and increased quality treatment
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
K2P Mentorship Program on Building Institutional Capacity on Evidence Informed Policy Making
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Doing embedded development and research – reflections on the start of the Results4TB programme
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Introductory Meeting on the project ‘Embedding Rapid Reviews in Health Policy-Making’
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Taavy Miller from University of North Carolina shares her internship experience
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Building Institutional Capacity for HPSR and Delivery Science- CIF is Europe region HUB
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Inter-regional workshop in preparation for transitioning towards domestic financing in TB, HIV and Malaria programmes
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Memorandum of Cooperation between the Health and Social Issues Committee of the Parliament of Georgia and Curatio International Foundation
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation at the Global Symposium on Health Systems Research
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The civil society gathered for the fourth time to discuss healthcare system challenges in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Project: HIV risk behavior among Men who have Sex with Men – Bio-Behavioral Surveillance Survey and Population Size Estimation
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Big Pharma Greed and Artificial Prices – Knocking on Door to Limit Access to HIV Medicines in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Civil society is gathering for the third time to hold a discussion about the healthcare
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
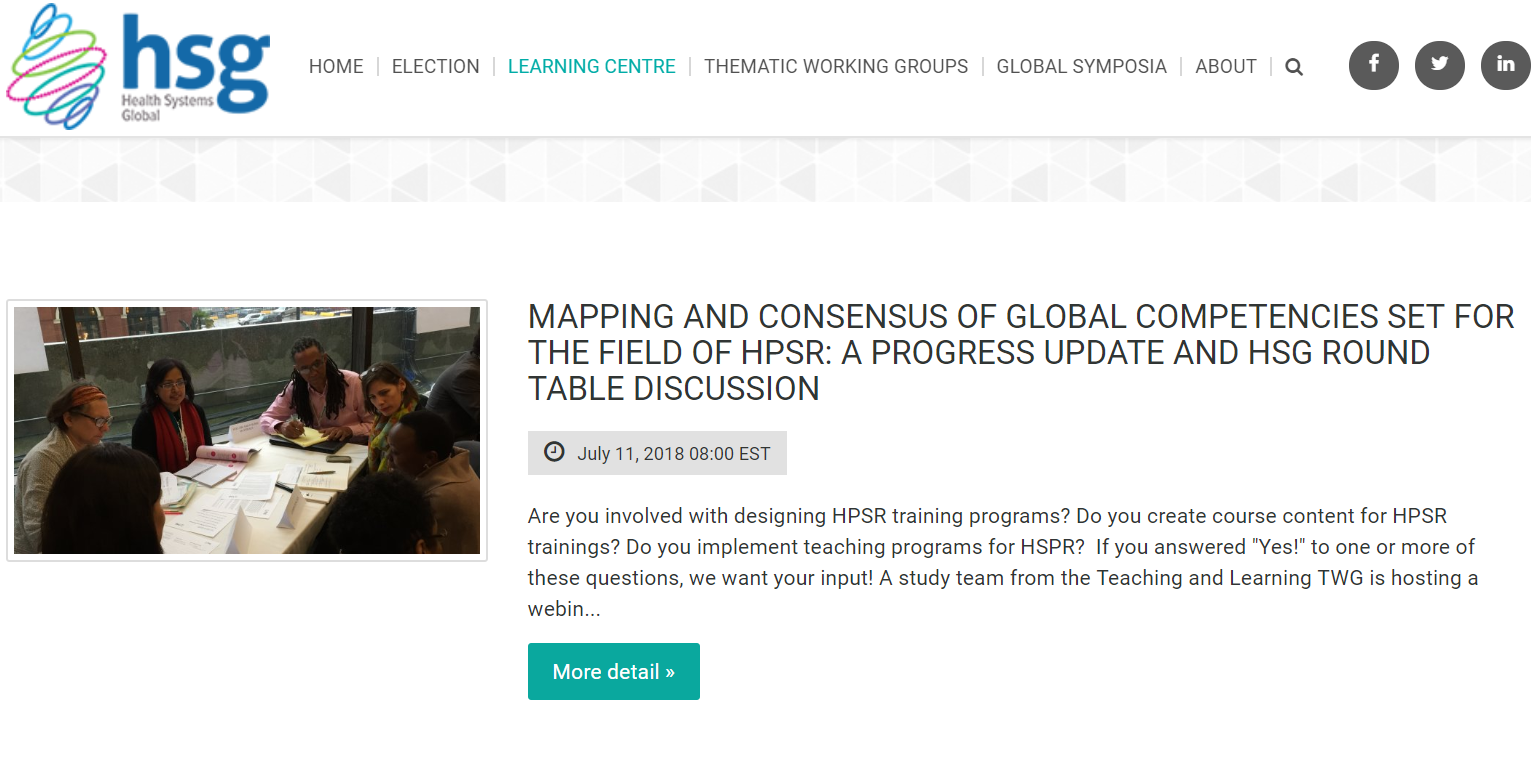
Webinar: Mapping and consensus of global competencies set for the field of HPSR: A progress update and HSG round table discussion
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Technical Assistance for evaluation of transition readiness and preparation of Transition and Sustainability Plan for Global Fund-supported programs in Tajikistan
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Technical Assistance for the preparation of Transition and Sustainability Plan for HIV program in Philippines
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
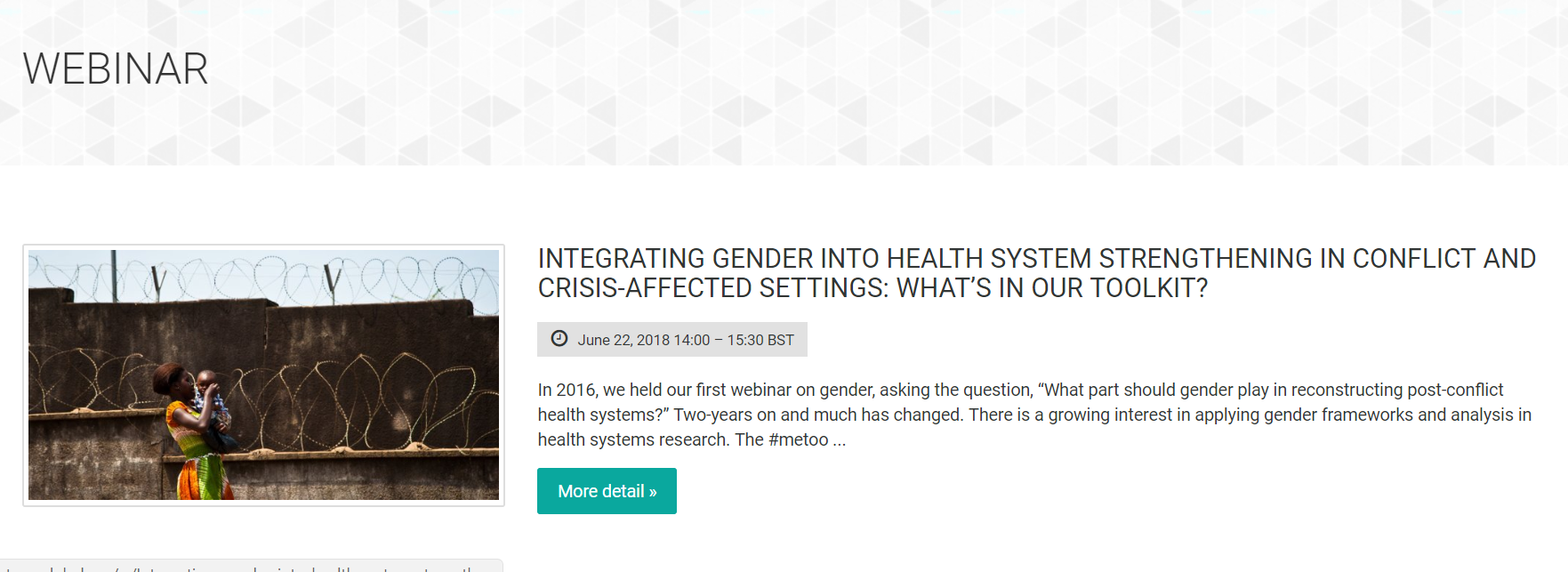
Webinar: Integrating gender into health system strengthening in conflict and crisis-affected settings; what’s in our toolkit?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Article: Barriers to mental health care utilization among internally displaced persons in the republic of Georgia: a rapid appraisal study
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
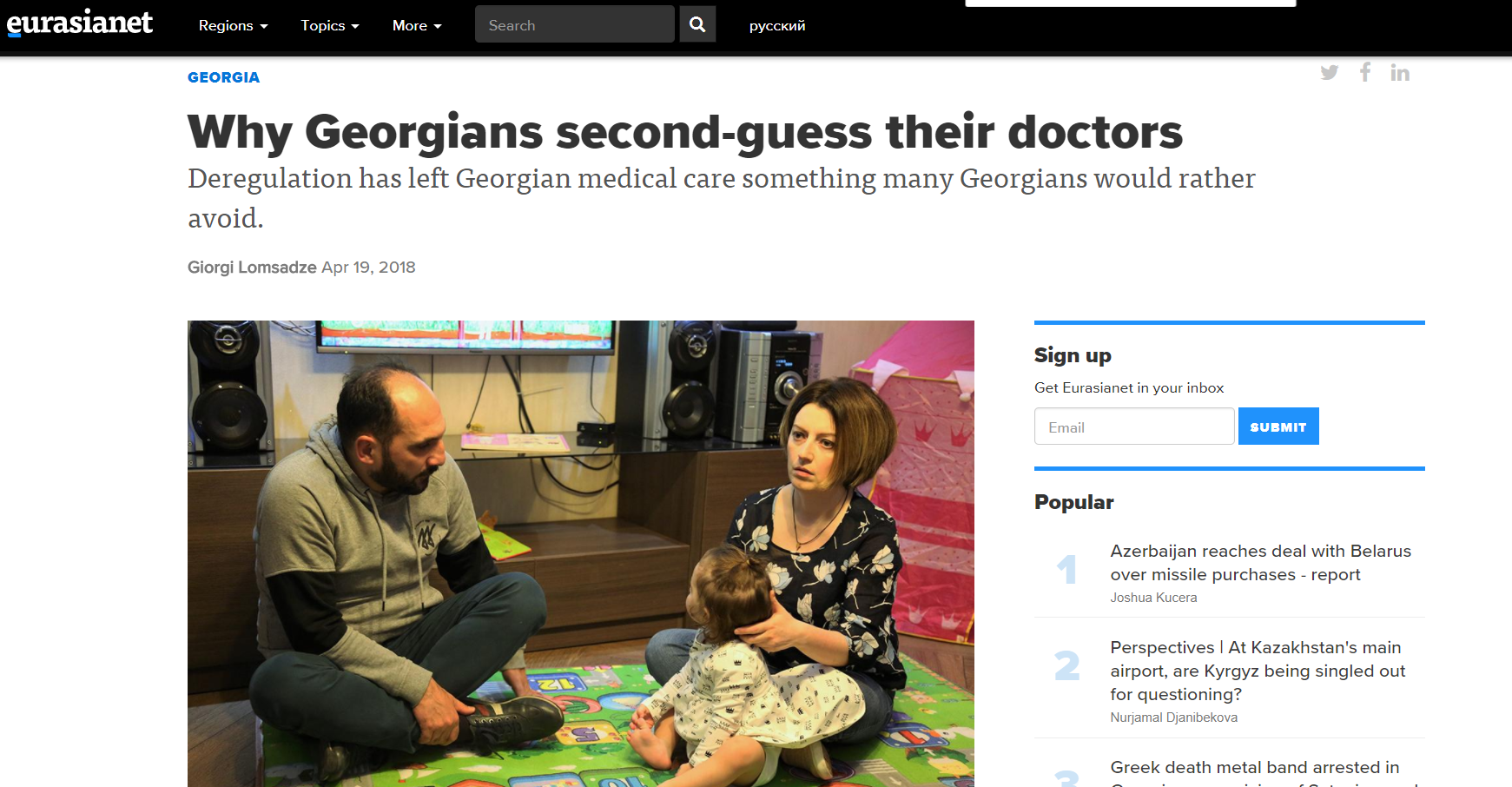
Why Georgians second-guess their doctors – Deregulation has left Georgian medical care something many Georgians would rather avoid
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Webinar on The peer review process – what happens when you send your manuscript to a journal
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Webinar on Improving Quality of Care during Childbirth: Learnings and Next Steps from the BetterBirth Trial
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Integrated Bio-behavioral surveillance and population size estimation survey among Female Sex Workers in Tbilisi and Batumi, Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Applying a Health Policy and Systems Research lens to Human Resources for Health: Capacity building, leadership and politics
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Empowering civil society for engagement in and monitoring the decision making in health sector in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation presented BBS and PSE study findings at the Civil Society Forum
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Article: Barriers to delivering mental health services in Georgia with an economic and financial focus: informing policy and acting on evidence
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The Interview on population size and Human Immunodeficiency Virus risk behaviors of People who Inject Drugs in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Population Size Estimation of People who Inject Drugs in Georgia 2016-2017
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
HIV risk and prevention behaviors among People Who Inject Drugs in seven cities of Georgia, 2017
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Conference paper: The Study of Barriers and Facilitators to Adherence to Treatment among Drug Resistant Tuberculosis Patients in Georgia to Inform Policy Decision
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Article: Human immunodeficiency virus prevalence and risk determinants among people who inject drugs in the Republic of Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Conference paper about realist evaluation: Informing policy, assessing its effects and understanding how it works for improved Tuberculosis management in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgian Healthcare and its Challenges: Healthcare Expert George Gotsadze will host the lecture
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
17 years in Curatio International Foundation: President Ketevan Chkhatarashvili to Leave Organization
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Article: Determinants analysis of outpatient service utilization in Georgia: can the approach help inform benefit package design?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Designing and evaluating provider results-based financing for tuberculosis care in Georgia (RBF4TB)
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Barriers and Facilitators to Adherence to Treatment Among Drug Resistant TB Patients in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation: Transition and Sustainability Portfolio
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Eastern Europe and Central Asia Regional Sustainability and Transition Coordination Summit 20-21 October, 2016 Vilnius, Lithuania
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Evaluation of UNICEF’s Contribution in Central and Eastern European Five Countries
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Washington DC hosts workshop Immunization Costing: what have we learned, can we do better?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Bio-Behavioral Surveillance Survey among Men who have Sex with Men in two major cities of Georgia, 2015
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
EPIC Studies – Governments Finance, On Average, More Than 50 Percent Of Immunization Expenses, 2010–11
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Bio-Behavioral Surveillance Survey among People Who Inject Drugs in 7 cities of Georgia, 2015
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
What can be done to improve treatment adherence among tuberculosis patients in Georgia: Looking through health systems lens
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
BioBehavior Surveillance Survey results were represented to the members of Parliament of Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF study results on 8th IAS Conference on HIV Pathogenesis, Treatment and Prevention
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Response to the “Final evaluation of GAVI support to Bosnia and Herzegovina”
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The drivers of facility-based immunization performance and costs. An application to Moldova
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Costs of routine immunization services in Moldova: Findings of a facility-based costing study
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Analyses of Costs and Financing of the Routine Immunization Program and New Vaccine Introduction in the Republic of Moldova
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Health Service Utilization for Mental, Behavioural and Emotional Problems among Conflict-Affected Population in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Healthcare Utilization and Expenditures for Chronic and Acute Conditions in Georgia: Does benefit package design matter?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation Hosts Health Systems Global Secretariat in Tbilisi, Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
An Impact Evaluation of Medical Insurance for Poor in Georgia: Preliminary Results and Policy Implications
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Georgian Healthcare System Barometer: Experts’ Evaluations of Changes Taking Place in the Healthcare
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The Forbes and Skoll World Forum to discuss HIV/AIDS Epidemic with Director of CIF
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Article on Springer-Determinants of Risky Sexual Behavior Among Injecting Drug Users in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Tobacco Use and Nicotine Dependence among Conflict-Affected Men in the Republic of Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
HIV prevalence and risk behaviors among key populations- Study Findings Published
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation Among Grant Management Solutions Awarded Partners
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation revealed the winner of its annual scholarship program
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Impact of global HIV/AIDS initiatives on health systems in Ukraine, Kyrgyzstan and Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Submission of Applications for CIF Scholarship for Master Program Students near to deadline
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Health care in Georgia is currently available for very rich and very poor
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Presentation of the findings of Assessment of Complex Non-Communicable Condition in Low Income Countries
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Contributing to publishing the paper: Circus monkeys or change agents? Civil society advocacy for HIV/AIDS in adverse policy environments
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
National Center for Biotechnology Information published CIF’s scientific paper on Unsafe injection and sexual risk behavior among injecting drug users in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Contribution to the development of National Health Care Strategy 2011-2015
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
New web guide for using qualitative approaches to health systems research
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF Study Published in BMC Magazine, The Role of Supportive Supervision on Immunization Program Outcome- a randomized filed trial from Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Releasing results of Bio-behavioral surveillance survey among men having sex with men
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Prices, Availability and Affordability of Medicines in Georgia-the New Study Report Endorsed
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Customer Satisfaction Research Report on Corporate Health Insurance Released
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
National and subnational HIV/AIDS coordination: are global health initiatives closing the gap between intent and practice?
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Internship at Curatio International Foundation is challenging for John Hopkins University Students
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF will Launch Fellowship for the Best Student of Healthcare/Public Health Management Faculty
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CoReform Project and the Ministry of Health Mark the Completion of the First Stage of Trainings on ICPC2 Application
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
First Stage of Training Course on Evidence Informed Policy Formulation Crowned
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The Study on System-wide Effects of the Global Fund on Georgia’s Health Care Systems posted on GHIN website
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Sentinel Surveillance Method to Provide Reliable HIV/AIDS Statistical Data
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Curatio International Foundation Contributes to Global HIV/AIDS Initiatives
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Mr. George Gotsadze approved as a Permanent Member of the Global Fund TRP
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The research article on Household Catastrophic Health Expenditure-evidence from Georgia and its policy implications published in BMC Health Services Research
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF Hosts workshop on Classifications for Hospital and Laboratory intervention
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF conducted a workshop to discuss HIV/AIDS Surveillance System Assessment results
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF conducted a workshop in the framework of the project funded by the Global Fund
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
The Global Fund Contracted Curatio International Foundation for Consulting Services
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
CIF and MoLHSA conduct a workshop on Integrated Model and Strategic Plan for the Health Information system development in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Dr. George Gotsadze – CIF director and PATH board member presented “Hope for health in a weakened nation”
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Natia Rukhadze – CIF Researcher at the Global HIV/AIDS Initiatives Network (GHIN) international workshop in Dublin, Ireland
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
George Gotsadze – CIF director at fifth Global NHA symposium in Lund, Sweden
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Yale University Announced Selection of Leading Georgian Public Health Expert, Ketevan Chkhatarashvili, as a 2007 Yale World Fellow Yale University announced the selection of the leading Georgian health policy advisor, Ketevan Chkhatarashvili, the preside
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Protocol of the Policy Club on the Public Health Organizational Development
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.
Final Report on Family Planning and Reproductive Health Assessment in Georgia
Former Soviet countries in the Eastern European and Central Asian (EECA) region are fighting the prevailing perception that their outdated hospital-based tuberculosis (TB) programs are failing to provide patient-centered care.














































































































































1 Comment. Leave new
Hi, I am Dr. Basharat from Pakistan here, associated with NTP for more than 16 years. You must be aware that Pakistan is a LMIC with more than 201 million population, with 150 districts and 1500 BMUs for provision of free TB care services in both public and private sector. Pakistan ranks 4th in both DS/ DR-TB among 30 HBCs globally. We started DOTS under NTP in 2001, integrated with PHC services in districts. Despite achieving 100% coverage in public sector health facilities and 20% contribution of TB case notified from private sector, we are yet to struggle for about 50% of missing/un-detected/un-diagnosed TB cases and static incidence at 270/100,000 since the MDGs era. We need to consider TB as socio-economic rather than a bio-medic phenomenon to be capable of achieving the SDGs and End TB targets, with a more holistic approach towards social determinants of TB. Having said that, I still believe that the secret of effective TB control to the level of elimination lies in community integrated and patient centered approach rather than a vertical one. I still believe that early diagnosis and complete treatment (cure not complete) is key towards elimination and prevention of drug resistance. Introduction of new diagnostics and treatment coupled with taking care of co-morbids (HIV+, diabetes and malnourished) and other key populations will add to success. In my view, no strategy would be better than community based approach (community workers and paramedic based) towards good control and elimination of TB. Thanks